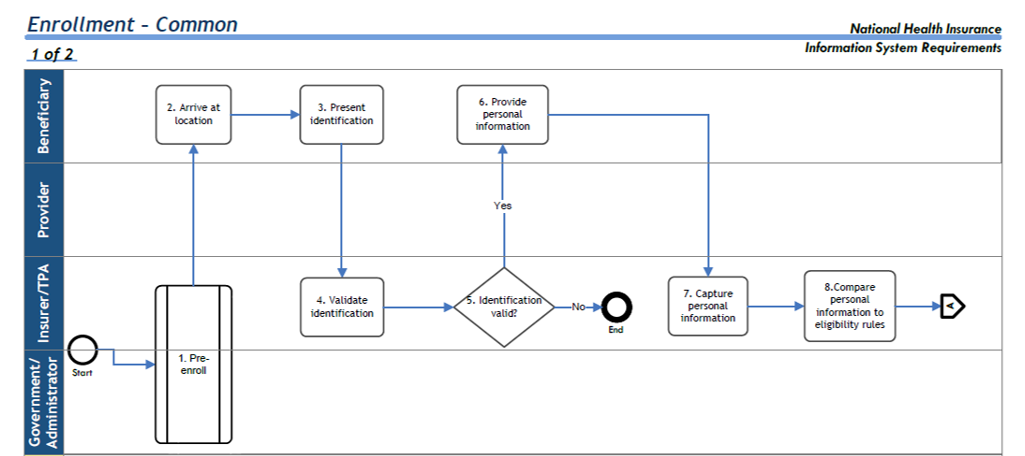
Process Group
Beneficiary Management
Objective
Verify identity and eligibility in a timely manner of persons seeking access to benefit plan services
Input
Demographics
Financial information
Geographic information
Qualifying criteria (see qualifying conditions)
Proof of identity (e.g., national identification card personal identification number, biometric information, photos)
Medical history
Current medical condition
Output
Time-based eligibility determination
Beneficiary identifier
Benefit plan number
Benefits class
Benefits plan detail
Feed into data repository
Task set
Validate identity documents
Record information in data repository
Measurable Outcomes
Eligibility is determined as approved or rejected.
Approved person receives proof of coverage (e.g. I.D. card)
Assign benefits class
Accurate list of beneficiary